Continuous respiratory rate monitoring to detect clinical deteriorations using wearable sensors
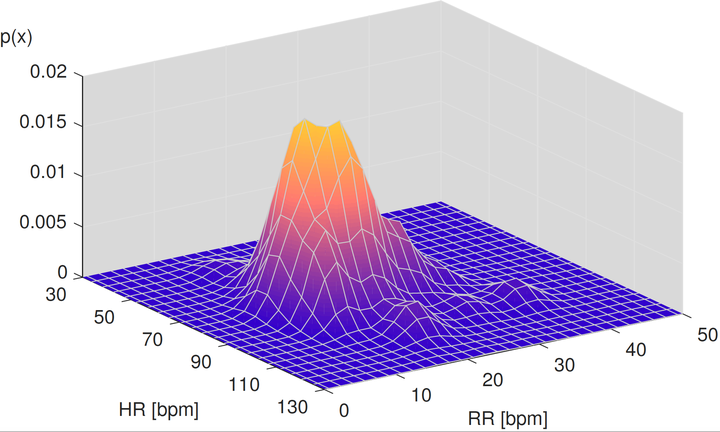 Image credit: P.H. Charlton (CC BY 4.0)
Image credit: P.H. Charlton (CC BY 4.0)
Abstract
Acutely-ill hospitalised patients are at risk of clinical deteriorations in health leading to adverse events such as cardiac arrests. Deteriorations are currently detected by manually measuring physiological parameters every 4-6 hours. Consequently, deteriorations can remain unrecognised between assessments, delaying clinical intervention. It may be possible to provide earlier detection of deteriorations by using wearable sensors for continuous physiological monitoring. Respiratory rate (RR) is not commonly monitored by wearable sensors, despite being a sensitive marker of deteriorations. This thesis presents investigations to identify an algorithm suitable for estimating RR from two signals commonly acquired by wearable sensors: the electrocardiogram (ECG) and photoplethysmogram (PPG). A suitable algorithm was then used to estimate RRs retrospectively from a physiological dataset acquired from acutely-ill patients to assess the potential utility of wearable sensors for detecting deteriorations. Existing RR algorithms were identified through a systematic review of the literature. A toolbox of RR algorithms was created to facilitate comprehensive assessments of algorithms across multiple datasets. This was used to assess the influence of technical and physiological factors on respiratory signals extracted from the ECG and PPG, providing recommendations for wearable sensor designs for RR estimation. An assessment of 95 RR algorithms using data from healthy and hospitalised patients showed that the algorithms did not perform well enough for use with acutely-ill patients. Therefore, a novel algorithm was designed specifically for use with wearable sensors, providing improved performance. The novel RR algorithm was used to estimate RRs retrospectively from wearable sensor data acquired from 184 patients. The performances of algorithms to detect deteriorations from the resulting wearable sensor data were similar to those used with routinely collected intermittent data, suggesting that it is feasible to use wearable sensors to continuously assess the likelihood of deterioration. However, the false alert rate increased when using wearable sensor data due to the continuous, rather than intermittent, monitoring. Therefore, further work is required to improve algorithms to detect deteriorations from wearable sensor data to provide clinically useful alerts.
Full text
- The published version is available here.